|
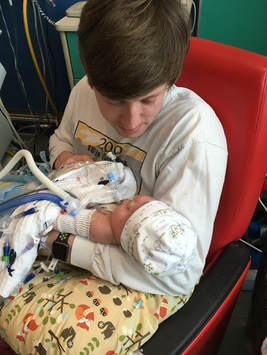
The last video we took of Will, sleeping peacefully, on February 27, 2018. Will was pretty stable the last few weeks of February. The doctors were making small tweaks to his medications, dialysis and ventilator but there were no big changes or surprises. A lot of time was spent talking about Will’s future and how we were going to move forward. The nephrologist thought that Will’s kidneys were most likely not going to start functioning, which seemed to be the biggest issue. He was probably going to need a kidney transplant, but he couldn’t be considered until he was about 22 pounds, at least a year. Maybe he would be in the PICU for that amount of time, waiting until he could be transferred and evaluated for a transplant. Maybe he would be able to come home and grow here, we didn’t know. The other concern was his heart. It was extremely weak in December, then we saw a big improvement as we entered the new year. After a few weeks his heart function got worse again, but still not as bad as it was at first. It seemed to be largely related to his fluid balance, but there was still the question of how much it would or could improve and if a heart transplant was potentially in his future as well. All of this talk about transplants and Will's future was full of so many unknowns not just for us but the doctors too. They didn’t know if he would even qualify based on many factors, mostly his brain bleed and the poor function off multiple organs. Plus he was a baby, which seemed to complicate everything even more. If he did qualify, we didn’t know if one of us would be a match for kidney donation and we didn’t even want to think about the details of him getting a heart. This path of transplants was one very real but uncertain direction for Will’s future. It seemed very overwhelming to me, but not unreachable. I would have done anything and everything to get Will whatever he needed to live. Most of the time I was just happy that they were talking in terms of the future and saying phrases like "at home nurse" and "in a few years..." Another, more positive and desirable path, was that Will’s kidneys would start working on their own. We were told that this was most likely not going to happen, that it would be a miracle. We had just seen miracle after miracle as Will continued to get better and Caroline came home, we have a big God and believed that He could do another miracle for Will. It seemed like if his kidneys would function on their own, even if just one could work enough to do it’s job, then the other things might fall into place. His heart might get stronger if it wasn’t fighting fluid overload and eventually his lungs could develop enough to remove the trach so he could breath on his own. Sometimes thinking about the best case scenario is the only thing that kept me going. I am a natural planner, I'm optimistic but realistic as well, and I imagined every possible situation and made it work in my mind. We prayed, we hoped and we wondered but we never expected an answer. We knew that Will would take the path God had laid out for him, regardless of how much I fought to find a solution. At the end of February I met with all of Will’s doctors, specialists and some nurses in charge of his care. We were discussing all these possible options and how to help Will keep getting better and grow while we waited to see what was going to happen. Misty came to the meeting. I have written about some of Will’s nurses who mean so much to us, but if you have been reading my posts you know that Misty is extremely special. I don’t know how to express what she means to us because there are no words that describe it. Misty was wonderful. She loved Will and she was there for me, she was there for all of us. She didn’t just listen to my concerns, answer my questions and chat about ordinary things to help distract me from the horrific reality going on around me - she did all those things - but she was really there. Completely present. When she was Will’s nurse we knew he was going to be taken care of above and beyond the standard of what was expected from any nurse. She not only made sure he was clean and comfortable, but she made sure his room felt calm and organized and fun. She made him CD’s with Disney lullabies and played movies for him. She dressed him and played with him and talked to him. Her job description included giving him medicine, monitoring his vitals and taking care of his physical needs . She did SO much more. She really cared. She didn’t have to come to this meeting, she came for Will, and she took notes and shared her concerns. She knew him better than any doctor. She spent 12-hour shift after 12-hour shift taking care of Will. After all the specialist talked and shared their ideas, concerns and plans, Misty interjected and I was relieved. At this point I was on the verge of a complete meltdown and I couldn’t say anything. I was just trying to get through the meeting so I could go into the bathroom and cry by myself. She spoke as a medical professional but she also was my voice, speaking every concern I wanted to bring up but couldn’t. She knew that Will was not himself. Over the past few days he had changed. He was swollen, uncomfortable, inconsolable at times. It was a different type of agitation. Not the kind of uncomfortable that was solved by a diaper change or switching positions. Will was a calm baby by nature, he was very low maintenance in the sense that he tolerated a lot, a lot more than can be expected of any human. The past few days it seemed like everything made him upset and he just couldn’t get settled down or comfortable. He hadn’t slept and his alert, kind little eyes seemed to be glazed over. Misty knew it and made sure everyone else knew too - something is wrong and we need to figure out what it is. On March 2, they started the process of exploring every possible reason as to why Will could be declining. More blood tests, samples taken and tests performed. Nothing came back that indicated a change. No positive cultures, no infection, no reason for this sudden decline. Theories were flying around everywhere but nothing pointed specifically to why he was suddenly deteriorating. One week ago he was making such good progress. One week ago I was giving him a few drops of milk from a bottle. One doctor told us he would never drink from a bottle and he did, eagerly. He was happy and sweet and we thought he was getting better. We were planning for his future. Now all of the sudden he was getting worse, they were adding support - more oxygen, epinephrine and norepinephrine to help his heart and re-starting medications that he hadn’t been needing since December. On March 3 I saw a twitch. No one thought it was a seizure. Doctors, nurses and the physician’s assistant all saw the twitching and they seemed to be confused by it and said maybe it had to do with electrolyte imbalance but it didn’t look like any typical seizure. They put an EEG on just to make sure. Not long after we discovered that it was a seizure, but not just a seizure. Will’s brain was having multiple seizures, sometimes at the same time, coming from areas all over his brain. I got the strong sense that it was something none of the doctors had really seen before or at least not frequently. He got a large dose of anti-seizure medication but that didn’t stop them. They added a drip of a second anti-seizure medication and were still having a hard time squelching them out. I remember standing at the EEG screen with the neurologist and he was showing me spikes where Will’s brain was trying to have a seizure. They were unstoppable and consuming every part of his brain. He was in a comatose state, sedated by multiple potent anti-seizure medications that weren’t doing their job. In my mind it felt like his brain’s way of shutting down, like it was misfiring from every location because his body was trying to die and we weren’t “letting” him. On March 4, the doctors started increasing the dose of epinephrine. It was referred to as a “rescue medication” because without it Will’s heart was not strong enough to pump blood throughout his body on it’s own. We changed his code, Do Not Resuscitate. There was no doubt that he was getting weaker by the hour and there was still no other explanation - all cultures, all tests continued to come back negative. The seizures were still happening, even with all the anti-seizure medications flooding his little body. He was sedated so there were no more signs of visual seizures but he was still on the EEG so they knew that he was still having them. He was just laying there peacefully, the ventilator doing most of his breathing and the epinephrine helping his heart beat. That night I was at Will’s bedside with the PA. He was one of the people who I had asked a billion questions to and knew Will very well. After I asked everything I could think of, I paused and through choked back tears I said, “This is a really hard question to ask, but do you think Will is trying to die and we won’t let him.” I think the question may have shocked him a little bit, but he kind of shrugged it off, “I don’t know, maybe” and left the room. On March 5 they added a third anti-seizure medication which basically put Will into a coma. I knew what was happening, I think everyone else did too, but no one really wanted to say it this time. In December it seemed like almost every doctor that discussed Will’s prognosis with us thought the best choice was to remove his support and hold him until he passed. In December there was so much confidence that he really had no chance but he made it through. He survived against every odd thrown against him. Now there was a sense that everyone knew that he was deteriorating quickly but no one really wanted to say it. I think it’s because no one wanted to admit it was reality. Everyone had grown so attached to him. In December he was just a patient, “Baby A.” Now he was Will. He had an identity and a personality and every doctor and nurse there had memories and experiences with him. I could tell in their demeanor and in their voices that they knew there was no coming back from this. Every organ system was simultaneously shutting down despite our best efforts to help him. When I walked into his room on the morning of March 6, it was like he was already gone. I was hit with overwhelming clarity and looking back I think it was God’s Spirit giving me peace that Will was already with him. Now it was my turn to fully hand him over. Almost like I was selfishly holding his one little hand and I needed to let go so that Will could go with Jesus and fully be healed. I wanted to hold on to him so badly. He was mine and I wanted him. I still do. I didn’t know how this could be happening, he was doing so much better, he was so sweet and just a perfect little boy. I didn’t want it to be true but for Will’s sake, I had to be willing to let go. I talked to everyone, waiting for someone to tell me that he could recover. I sought out every optimistic doctor I knew but never found the hope I was looking for. God made him and he belonged to God but God gave him to me, he was mine. Nothing about it seemed fair or right. How could I just let him continue to sit up here hooked up to all those machines that were making his body work. How could I let him endure this suffering just because I couldn’t say good bye. I was determined to just let him ride it out, maybe he could overcome it just like he had a few months before. Maybe it was just a setback. I kept waiting for someone to confirm it and give me permission to hold on. But then I heard something that scared me. One of Will’s nurses said that we could just keep him up here like this forever. Forever. So he just lives here, in a coma, with a machine making him breath and medication making his heart beat and dialysis doing all the work of his kidneys and his brain seizing almost continually. We made the most difficult decision to stop rescuing Will. This is not a life. “This is not a life.” These are the words that one of Will’s doctors said to me that afternoon when he came in to say goodbye. That afternoon we had a stream of people - doctors, nurses, therapists - come in to say goodbye to Will. There were a lot of tears, many thoughtful and heartfelt words but aside from Will’s nurse, Misty, this doctor gave the most genuine and sincere goodbye of them all. He came in already in tears. Just that image of seeing an ICU doctor in tears is something I thought I would never experience. They all seem so tough and calloused and withdrawn. They have to be. He sat down across from me, my precious baby boy dying in my arms, and said how his prayers have changed, how this is not a life for any child. He kissed my boy, looked me in the eye and squeezed my mom’s hand. It was heartfelt and genuine, a moment I will remember forever. Taylor and I spent that day holding our baby for the last time. Caroline, his twin sister, was with him all day, exactly as she should be. He passed away in my arms around 9pm. "It's a Small World" lullaby was softly playing in the background and I felt his body let out it's last breath here on Earth. I asked them to turn the monitors away and I didn't know if I would know the moment when he took his last breath. I did and it's a moment that will haunt me forever. We dressed him, wrapped him in a blanket, laid him in a little woven basket and said an impossible goodbye. We will never be the same again. Taylor and Will on March 6. My last picture of Will, taken on March 6, 2018.
4 Comments
Jenny
9/11/2018 06:20:05 pm
You are so brave to share your story and such an incredible mom. It's an honor to read your words and see how Jesus gave you the comfort you needed in the moment you needed it, and I pray for a lifetime of that as you continue to long for your son.
Reply
Courtney Hughes
9/11/2018 07:46:45 pm
Thank you, Jenny! That is so kind!
Reply
Deena
9/13/2018 04:09:31 pm
I’ve intentionally put off reading this until I could “be ready”. Impossible to ever be ready for anything like this. You write so beautifully and manage to turn total darkness into bright light. Thinking of you all always🙏🙏
Reply
Courtney Hughes
9/14/2018 04:28:36 pm
Thank you so much Deena! You are always so encouraging and thoughtful and I am always so touched by your comments ❤️
Reply
Leave a Reply. |
Our MissionOur mission is to children from developing countries receiving heart treatment in Jacksonville, FL. Archives
January 2023
AuthorMy name is Courtney Hughes and I am Will's mommy. I am happy that you are here to read Will's story and make a difference with us! |