|
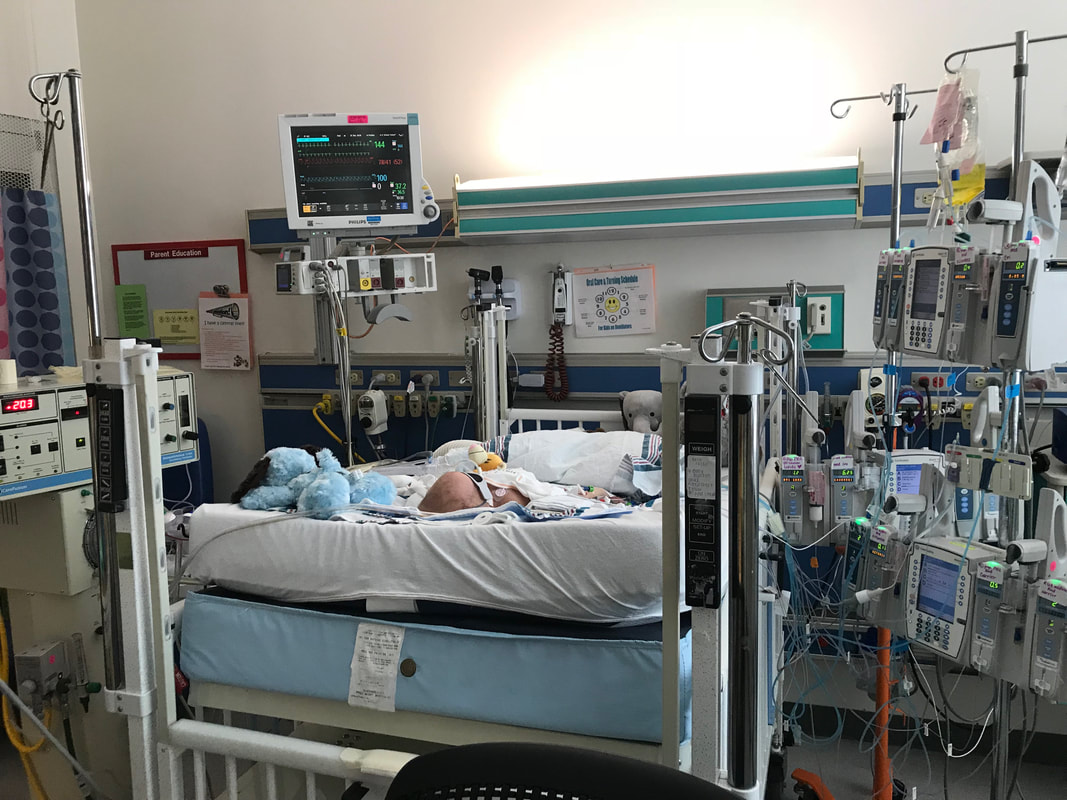
Extracorporeal Membrane Oxygenation. Hearing that your child needs to be on this machine, also know as ECMO, is not what you want to hear. I had never heard of this machine before, but on December 11 the doctors told us that Will needed to be put on ECMO or his chances of making it even a few more days was pretty much none. This machine is used for patients with life-threatening heart and/or lung problems. There is a large plastic tube inserted into the blood vessel in the patient’s neck which takes the blood out of the heart and into the ECMO machine. The machine oxygenates and cleans the blood before it is pumped back into the body. When successful, ECMO will help support a patient while doctors can treat the underlying problem and it can be a life-saving machine. However, like with anything, there are risks. On the morning of December 10 neither baby was showing any signs of improvement. Caroline was in critical condition after the pulmonary hemorrhage and we still had no test results indicating why they were so sick. Caroline was on an oscillator and Will on a ventilator for respiratory support and both of them had very poor heart function. They both had enlarged livers, poor kidney function and Will also had an enlarged spleen. Both babies were starting to swell due to poor kidney function but Will was retaining more fluid than his sister. That night the doctor put a catheter in his stomach to help draw out more fluid. We were told that if they didn’t put the catheter in he may not make it a few more days because the extra fluid puts pressure on his heart, which was already weak, and on his lungs, making it harder to breath. Will had a really hard time overnight. He stopped draining through the catheter, his kidneys stopped producing any urine and his heart was not squeezing well. I had spent the night at my parent’s house with our two older children and this is the text I got from Taylor when I woke up in the morning, “He (the doctor) just told me he is extremely concerned for Will and doesn’t want us to be blindsided if something happens. Just get here as soon as you can, the doctor said if he goes into a heart arrhythmia or if his heart stops he doesn't know that they can get it going again.” Two days before I thought I would show up to the hospital to find that my daughter was gone, today it was my son. On December 11, the doctors started talking about putting Will on ECMO. It was the only thing that the PICU team thought would give him a chance, even if it was a small chance. The procedure to insert the tubes and begin the process went smoothly and we had great hope that this would give his little body the chance to rest and recover. When your child is on ECMO, there are a lot of people, medications and equipment involved. There is a PICU nurse and an ECMO nurse present at all times in the room. Will’s first few hours on ECMO went well, he was responding to the machine and everything was working the way it was supposed to. Then he had a head ultrasound. One of the major risks with ECMO is bleeding, especially for little babies. The patient needs a large dose of blood thinner for the process to work and Will was already having issues with his blood coagulating correctly. The head ultrasound showed that his brain was bleeding. I was sitting with Will on the night of December 12. His bed was raised up high, so I had gotten an office chair that the nurses use and adjusted it up to the highest position so I could sit next to the bed and hold his hand. That night Taylor had gone to our daughter’s Christmas performance so I was alone with the babies and was planning to go back to my parents' house when Taylor got back from the show. Will’s room was positioned at the end of the hallway and I remember glancing over to see Taylor coming down the hallway. He wasn’t supposed to be back for a few hours and I immediately got huge lump in my throat. I knew something was wrong. Without even saying hello I blurted out, “What are you doing here?” He acted surprised, like he thought I should know something that he didn’t. He told me that right as he arrived at the performance the hospital Chaplin had called him and said that the doctors needed to talk to us and he needed to come back. I had no idea that the Chaplin had called Taylor or that anything was wrong. Minutes later we were taken down the hallway to a meeting room and the whole team of doctors and nurses came in. They explained to us that Will had to come off ECMO because of the brain bleed. He had been on it less than 24-hours and the positive effects of ECMO had not even begun to take effect. The doctor thought that Will may have a short time after being taken off the machine, but made it very clear to us that either his heart would stop or his lungs would collapse within a few minutes or hours. There was nothing else they could do. Everyone left the room and prepared to disconnect Will from ECMO as we crumbled, completely devastated. Taylor and I were both sobbing and I remember thinking so many things but all I could say was, “I don’t want him to die.” After a few minutes alone, we went back to Will’s room to be with our baby for what we thought were going to be his last few minutes, possibly hours, on Earth. I pulled the tall chair back up to the bed to hold his hand and Taylor stood next to me near his head. Through blurry eyes I kept glancing at the monitor then back down at Will. Lots for doctors and nurses were gathered in our room doing the same thing. After about thirty minutes I asked the doctor when they were going to disconnect him from ECMO. “He’s all on his own,” he replied, keeping his eyes fixed on the monitor. It felt like everyone was just waiting for him to die, there was a certainty that it would happen any minute. But as the minutes went past, the room got more and more empty. Will’s heart never stopped that night, it kept going the next day and the next and for almost seven more weeks after that. His lungs never collapsed, ever. No one could believe it. It was a miracle. He is a miracle. A few weeks later I was talking to the same doctor who was there that night and he brought up some things that he thought Will would never be able to do. Will was doing fairly well at that point, he was pretty stable and just needed time to grow and get stronger until we could see what his path was going to be. The doctor was mentioning things like Will would probably never drink from a bottle and he may never walk or talk, all things that were unknown and far into the future. I reminded him that Will had already done a lot of things that no one thought he could, specifically he lived through something that no one thought he would. He replied saying that it just goes to show how little control we have. We feel like we are in control with all the medication and equipment and support available, but really, even with all the things we can control, we are totally out of control. Even with all the medical support possible, God could have taken Will despite all of our efforts. God could also keep his heart beating despite all of the reasons why it shouldn’t. He is the Creator and Giver of life. That night He gave Will life. He gave us seven more weeks to spend with our baby. He gave us hope. He gave us a miracle. This is what Will's room looked like after he was taken off ECMO. The large machine on the left is the oscillator, which he was on for respiratory support. The black screen mounted on the wall is the monitor that we were constantly looking at that night to watch his heart rate and blood pressure as we were waiting to see if they would start dropping. On the right are two IV poles with medication drips going into Will's PICC lines, he had one in his leg and one in his arm at this point because he required so many medications. You can tell that his head is swollen from the top as was the rest of his body.
0 Comments
Leave a Reply. |
Our MissionOur mission is to children from developing countries receiving heart treatment in Jacksonville, FL. Archives
January 2023
AuthorMy name is Courtney Hughes and I am Will's mommy. I am happy that you are here to read Will's story and make a difference with us! |