|
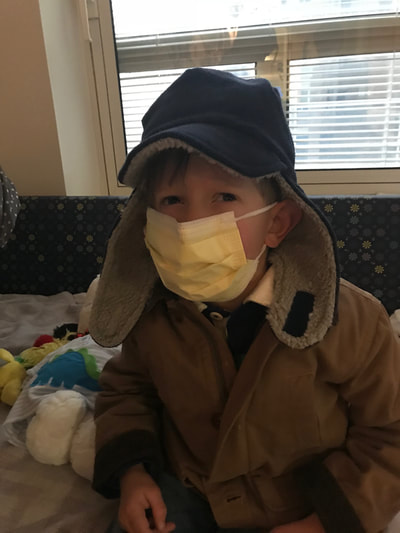
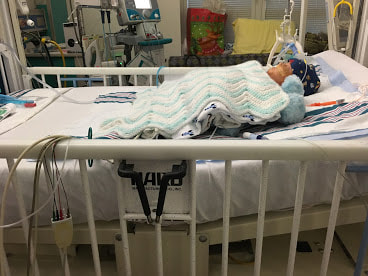
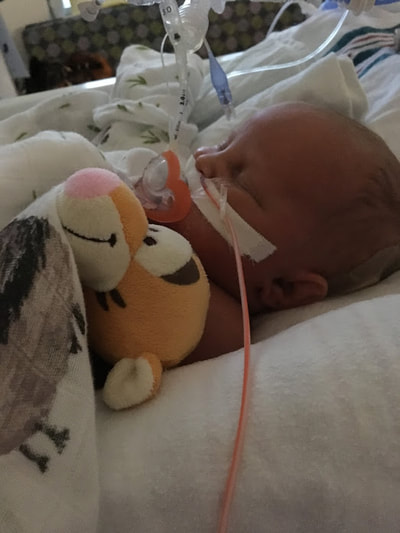
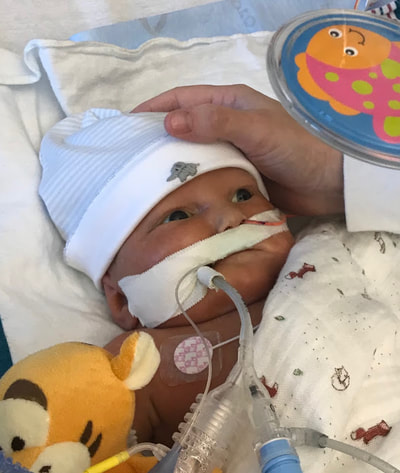
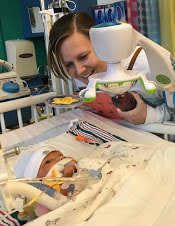
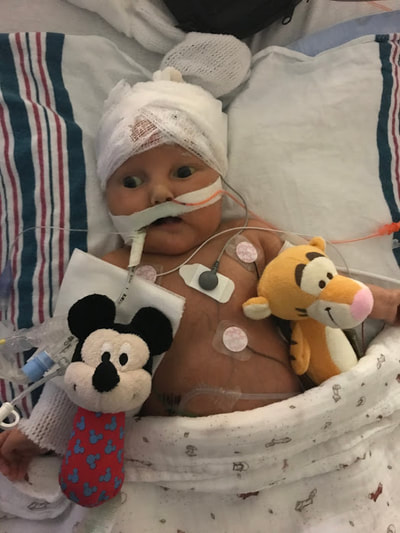
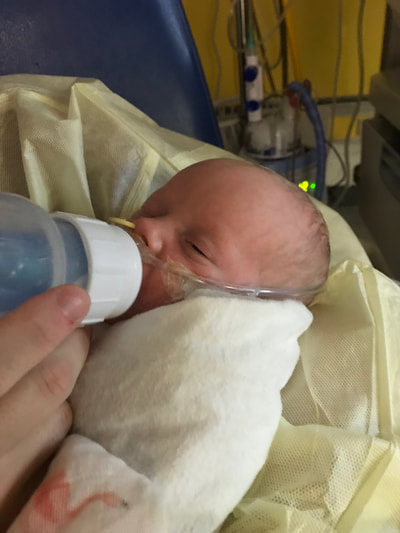
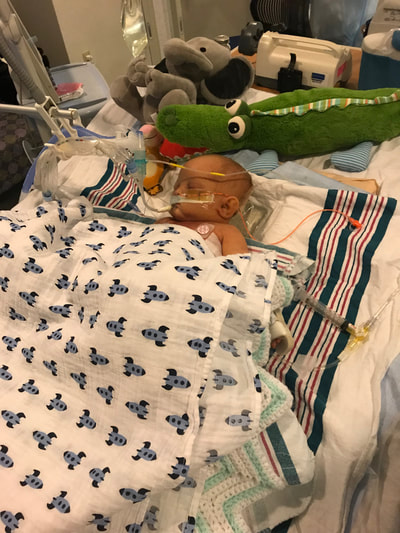
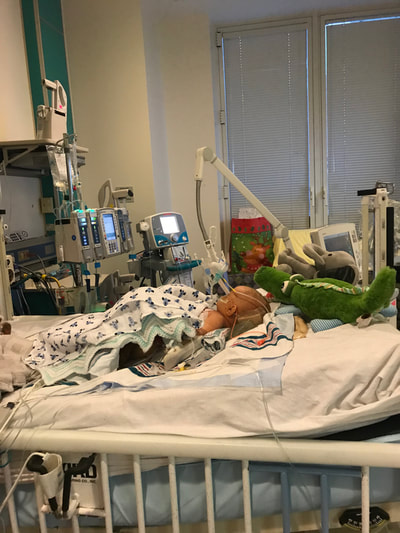
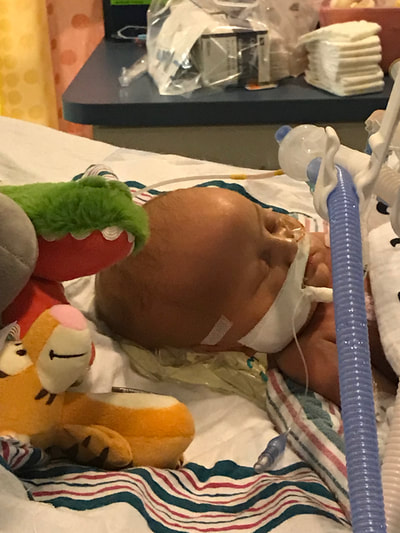
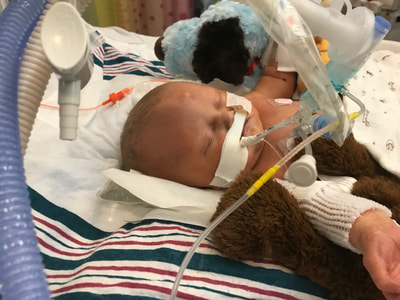
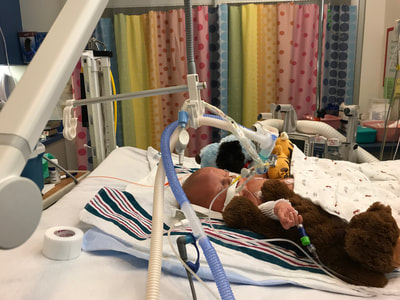
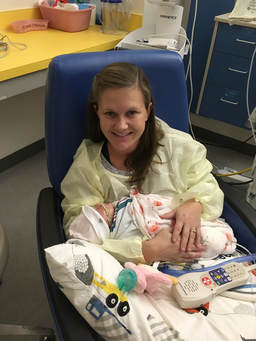
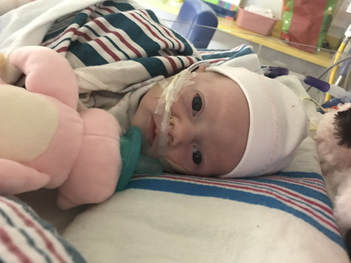
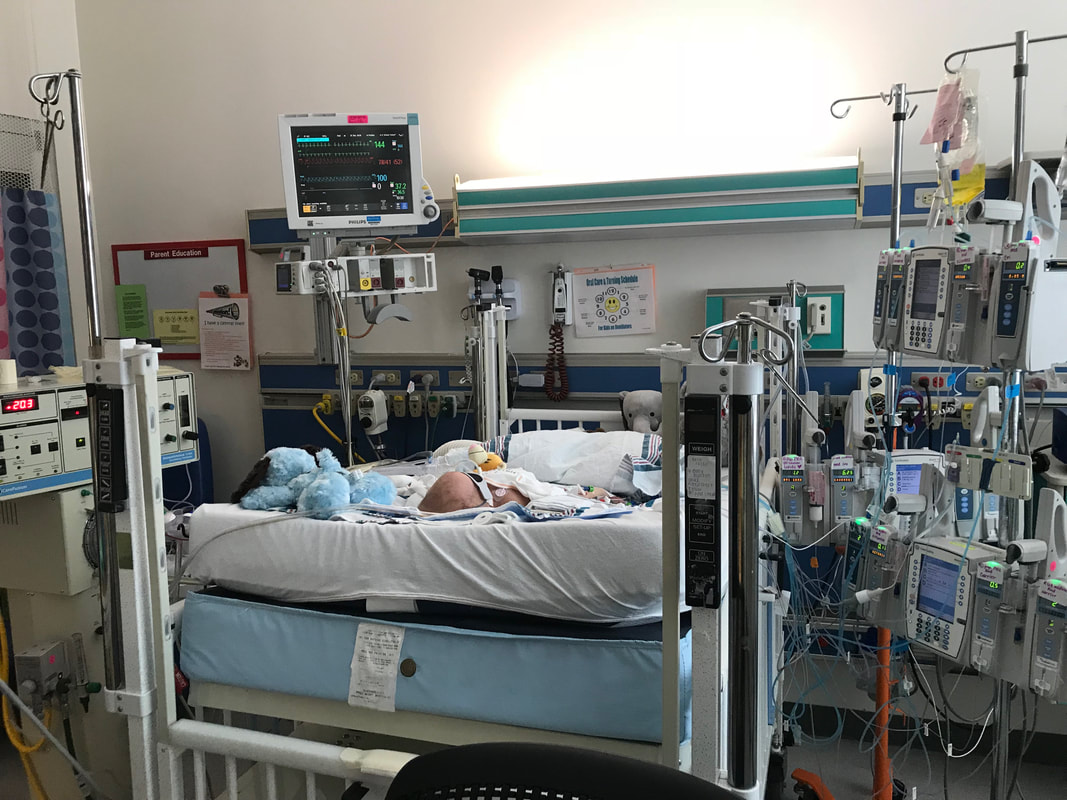
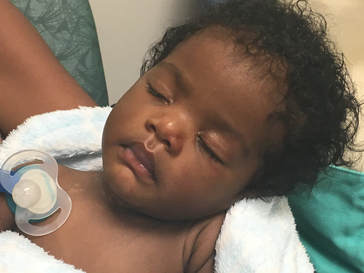
Taylor and I spent the last few days of 2017 preparing for a huge transition for our family. Caroline was on the hospital floor preparing to come home. She was weaning off one last medication and was being monitored to make sure she was gaining weight properly. She had all her final testing done, she had learned to nurse and was acting just like a normal baby. On December 31, Caroline and Will’s due date, we were told that Caroline could go home the next day. The first emotions were joy, excitement and happiness. Our baby girl stayed in the hospital for 27 days and taking her home completely recovered and healthy was the best possible outcome. But then came fear. She had so many monitors on at the hospital, how would I know if something was wrong? What if she stopped eating or her temperature was low or her heart started to get weak again? What if she got sick again? What if she got exposed to another virus or bacteria? It was scary to take her home. Leaving the hospital felt almost like a crime. Like we were stealing her or something. She had been there for what seemed like such a long time and we just walked out with her, put her in the car and left, just like that. January 1st was a cold, rainy day. Caroline's Grandaddy and big brother came to get her in the afternoon. It was one day after her original due date, so in a way it was exactly when she was supposed to be coming home - right on schedule. I spent some time with Will that day and then my dad stayed with him while Taylor took me, Joshua and Caroline home. He helped me get everything set up, made sure we had everything we needed and then headed back to the hospital. Since I was nursing, I obviously had to be with Caroline through the night and Taylor stayed at the hospital every night with Will. I am thankful that Will never spent a night alone and I would never ever change that, but being by myself with a fragile newborn that almost died was very daunting. It's hard to describe what I felt like when Taylor left, maybe lonely or helpless or scared or sad, I'm not really sure. All I know is that Will having his daddy there with him through the night was a top priority for us, so in a way I didn't acknowledge any of those feelings or fear and instead just moved forward. Having a healthy newborn is a lot to handle, a lot of learning, a lot of adjusting - the sleepless nights, nursing every few hours, rocking, soothing, swaying. With our two older children, I had Taylor home to help me. Not now. Now I was alone, completely and totally responsible for Caroline. I was up with her all night the first few weeks. There were multiple times we both sat on the couch, crying through the late hours of the night. I was scared I would fall asleep holding her, but she didn’t want to be put down and I didn't want to put her down. She was catching up from lost time in the hospital, so she was eating every 2 hours. Every time she cried I was scared she would stop breathing or work herself up like the day she had the pulmonary hemorrhage. Every time I gave her a bath or changed her diaper or put a new outfit on her she screamed. Apparently this is common for babies who have been in the hospital for a long time. "Touch-me-not" is what the occupational therapist called her. She didn’t want to be touched because every time she was touched in the hospital it was unpleasant. Someone was poking her with a needle or sticking something in her nose or mouth. Caroline wasn’t used to being touched in a loving, gentle way and every time I touched her (unless I was simply holding her) her whole body would turn red and she would scream and cry. Thankfully I was pretty much recovered from my c-section at this point, but there were still things that were hard for me to do by myself. Standing for hours and bouncing her hurt. Bending over the tub to give her a bath was still uncomfortable. On top of how physically difficult that first month was, the emotional pain was hard as well. It was the guilt, the sadness, the fear, a constant state of balancing and stress and survival. I felt guilty that I couldn’t have both of our older children come home. I still wasn’t supposed to lift my one year old, so if she was home I needed someone with me to help and watch her. Most nights she spent the night at my mom and dad’s house because I just couldn’t take care of all three children by myself. A mother is supposed to be able to take care of her children, I couldn't and it felt like a failure. I felt guilty leaving Caroline with Taylor during the day so I could go see Will. Caroline knew how to drink from a bottle but she preferred to nurse, so every day she had to have one or two bottles with Taylor while I was gone and I felt bad for leaving her. I felt bad for not letting her nurse for every feeding after she had worked so hard to learn how to. I felt like I couldn’t give my older two children enough attention, like I was neglecting them in some way. Most of all, I hated not being with Will every second. I usually got 5-6 hours per day with him. Depending on the day I sometimes got to hold him or help with a bath or watch him do therapy. But sometimes he had to have a procedure or he was asleep or I needed to talk to doctors and I didn’t get a chance to hold him or play with him. Sometimes those 5-6 hours flew by and I left feeling like I missed out on an entire day with him. When I got home my mind was there and when I was with Will my mind was at home. I felt like I couldn’t be all in or fully present. I felt guilty about that too. Even though I know there is nothing I could have done better or differently, that's just how I felt, nothing I did could have changed those feelings. While January was a very difficult month, I was constantly reminded of what a miracle Caroline is. It sometimes got overlooked because we were so focused on Will and helping him get better, but I was reminded the day before we went home while talking to the cardiologist that Caroline's story "should" have been completely different. She told me that many of the doctors didn’t think either of them would recover. I remember thinking how amazing that Caroline did. She and her brother had the same virus and while he was still in critical condition, she was coming home. It was amazing but how could that be? How could it affect them so differently? How could one recover and the other not? Now that Will is gone, her recovery is even more miraculous to me. There are so many times I look at her and just think how amazing that she had the same virus that made her brother so sick and took his life. How amazing that she is here with us. When Caroline left the hospital Will was still in critical condition but slightly improving. The dialysis was working well enough that while he was still swollen, he had started getting some fluid off. Every day he seemed to be more alert, looking around, moving his arms and even crying. Watching a baby cry while intubated is very strange because you can’t hear anything. You see them cry, mouth open, tears flowing but no sound. Seeing Will cry was heartbreaking because I couldn’t just pick him up and comfort him like I would with Caroline. Seeing Will cry was also weirdly encouraging. He was doing something that normal babies do. He was responding and reacting. On January 3 Will went to surgery to get a dialysis catheter. Having the correct catheter to do peritoneal dialysis helped the whole process to work much better. Sending Will off to surgery was scary, mostly because weeks before the surgeon told us he would bleed to death if he underwent this procedure. Thankfully, we met a different surgeon who does the procedure in a completely different way, so there was less risk of bleeding and he was confident that if Will did start bleeding it would be a small amount and he could stop it. The procedure went well and the catheter worked well. We were hoping that his kidneys would start working and he wouldn’t need the dialysis for long. We were hoping he wouldn’t need a kidney transplant and even if his kidneys didn’t function at 100% that they would work enough for him to get by (at least for a while) without continuous dialysis until he was big enough for a transplant. At this point we were just waiting to see what Will’s path was going to be. We were starting off 2018 with a lot of hope for Will. We didn’t know what the future held, but we were positive and it seemed like a lot of the doctors and nurses started to be more positive as well. Will had made it through when no one thought he would make it to the end of the year and we had every expectation that he would keep going in that direction. Will with his paci! Nurse Ashley cut Caroline and Will's pacis so they could have them while intubated - we love her and we love watching our sweet boy enjoy his paci!
0 Comments
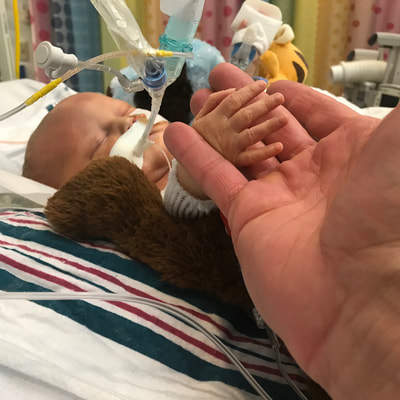
Some of Caroline's last days in the PICU. December 26 was a big day for both babies. A turning point. Taylor sent a very long text that morning after rounds. Our favorite doctor, the one I am always praising, was there that day. Taylor said, “The doctor is making moves. Caroline is coming off the nasal flow and will be breathing completely on her own today. He wants her feeding through a bottle every 2-3 hours and getting whatever she doesn’t take through the feeding tube. She’s going to wean completely off phentynal (a narcotic) and he wants her out of the PICU as soon as possible. He thinks the oscillator is no longer helping Will. He doesn’t want to keep him paralyzed anymore so they are going to put him on a ventilator today. The catheter is causing too many problems and since the surgeon won’t place a dialysis catheter he is going to change out the catheter himself. Will is also going to get a feeding tube and start slowly at 2mls per hour. He said that Will needs to try to move forward if he is going to get better.” This is a doctor who was willing to give our baby a chance, not just write him off as being potentially neurological damaged or irreversibly sick. So we moved forward. Will's room at the end of December. A few nights before I had talked to the surgeon about replacing the catheter with a true dialysis catheter. He didn’t think it was possible and I was devastated as I felt like dialysis was his only hope. If he couldn’t get fluid off and properly filtrate his blood, there was no chance for him to recover. The current catheter wasn’t working and the correct catheter could not be put in because the surgeon thought he would bleed to death during surgery, so the only reasonable option was to replace the current catheter with another one in a non-surgical procedure done at his bedside. I remember sitting in a chair in Caroline’s room holding her and I was facing the sliding glass door between her and Will’s room. The nurses prepared everything they needed to switch out the catheter. This still wasn’t the correct dialysis catheter, but it was one that should work better than what he had. I watched as the doctor and multiple nurses gathered around his bed to do this procedure. I felt helpless, anxious, sacred. I knew there was a very good chance that I could be getting ready to watch my baby boy experience some catastrophic event or even die. I knew there was a chance he could start bleeding and they wouldn’t be able to control it. I knew there was a chance doing this procedure would be too much on him and his heart would stop. I just sat there, holding Caroline, with all these thoughts racing through my mind. The charge nurse kindly stood between the rooms and updated me on the progress of the procedure. I heard their conversation, the doctor asking for this and that, and not really understanding any of it. Finally the nurse said that it seemed like everything went well. I was relieved but only for a little while. Later that day they switched Will from the oscillator to the ventilator. The actual switch was terrifying but he made it over, still breathing. But could he maintain it? Could he take breaths on his own? What if he had to go back to the oscillator? Would there be any path for him? Only time would tell and we continued living hour to hour - every cycle of dialysis, every minute he kept breathing on the ventilator. One of the positive aspects of coming off the oscillator was that he no longer had to be paralyzed and could start moving around again. That day had a lot of moments when we were just holding our breath, waiting to see what would happen and wondering if our baby would survive. It was hard. It was also hard that night when Caroline left to go to the hospital floor. I have never felt such mixed emotions. I was so happy that she was getting out of the PICU. It meant that she was recovering, she was going to survive and probably be at home soon. But he was staying. She was leaving her brother behind and I didn’t know if they would ever see each other again. She knew him the best, they spent the most time together. They heard each other’s heart beats, kicked each other and were born only one minute apart from each other. They were separated in the PICU, but still close to each other and now she was going away. I asked the nurse if I could take her into his room to say good bye. She graciously helped me wheel Caroline’s IV pole and portable oxygen into Will’s room. I laid her on his bed and cried. They were so perfect and I knew that it was very possible that it was the last time I would ever see them together. I placed her back in her bed, told Will goodnight and pulled a red wagon full of all Caroline’s things up to another room on another floor. It was sad and happy. That walk out of the PICU felt victorious in a way but at the same time it just didn’t feel right. The life we planned for them was together, not apart. There was still so much that was unknown but so much to celebrate. I spent the night with Caroline and Taylor stayed with Will, just like our first night at the hospital. Caroline was up all night, practicing drinking from a bottle and getting through her withdraw symptoms. Will had a lot to prove that night. Caroline in her new room on the hospital floor. She was weaned off oxygen and all breathing support. She got her feeding tube removed once she was taking full feeds from a bottle consistently and weaned off all her medications. We spent a lot of time helping her learn to eat and holding her. The next morning, December 27, Will got a feeding tube and started getting 1ml of breastmilk per hour. After weeks of feeling like I could do nothing to help my baby, seeing him with a feeding tube was wonderful. All those hours of pumping were paying off and I could do at least one thing to help him get better. He weaned down on the epinephrine drip, the medication that was helping his heart continue to pump, got to a very low dose and eventually completely off. Since his paralytic was stopped the day before, he was now squeezing our finger, looking around and taking breaths on his own. He was maintaining a stable blood pressure and his heart function was improving. I was in Caroline’s room when the cardiologist came to talk to me about Will’s echo. She was amazed that his heart was improving. She said it went from severely depressed to mildly depressed and she had never seen a child with a heart as low functioning as his recover. She saw no reason why he wouldn’t be okay. Even if his heart didn’t improve anymore, she thought he would be fine - no heart procedure, surgery or transplant. The main issue now was his kidneys. Apparently kidneys are very resilient and they usually recover on their own, although it could take weeks or months for this to happen. Now that his heart function was better, they were pretty certain that his kidneys were receiving proper blood flow and it would hopefully just be a matter of time. We ended 2017 with so much hope. Caroline was on her way home and Will seemed to be getting better - recovering even. He was becoming more alert everyday and acting very appropriately for his age, despite the brain bleed. Our little boy had made it longer and further than anyone thought he would. This was the week when I started truly believing that Will would get better. I wasn’t delusional, I didn’t think he was right behind Caroline and I knew he had a very long way to go. I knew that there would be a lot more obstacles, procedures and potentially major surgeries to get him there. I thought he would most likely spend his first birthday in the hospital. I thought he may have to be moved to another hospital if he needed a transplant in the future. I knew he might have a disability, maybe even something severe. I knew he would likely be developmentally delayed and everything might be harder for him. I was aware that we would likely have a nurse in our home. We would have hours of therapy and have more doctors appointments than I could probably ever imagine. I knew it would be hard on our family and even change our lives, but for the better. He was our little boy and there is no obstacle, disability or complication that we weren’t willing to encounter. He was more than worth it. I really did think he would get better. I thought he would come home. Sweet Will in the beginning of 2018 - so much hope! To All the Nurses Who Loved Our Will, There are not words powerful enough to adequately thank you. I learned quickly that you - Pediatric ICU nurses - are a very special kind of nurse, a very special kind of person. I have tried to describe to people out here what you do everyday and my words always fail. An outsider can’t begin to understand the magnitude of your influence or importance of what you do until they have seen it in action. Your daily reality is foreign to most of us and even once we’ve had a glimpse into your world we cannot fully understand or appreciate all that you do for us and for our children. We watched you care for our baby in a way we could not. We watched you monitor Will’s numbers, administer medications, draw blood, send samples, manage IV drips and change dressings. We watched you bathe him, change his diapers and keep him warm. We watched you respond, rescue and resuscitate. We watched you advocate for him and speak up when you knew something was wrong. We watched you wait until 4pm to eat lunch because taking care of Will was more important than taking care of yourself. We watched as you put off pumping milk for your own baby another hour, another two hours, because Will needed your attention. We watched you create the most positive and peaceful environment possible for our little boy. We watched you play Disney movies and lullabies so his room full of monitors and beeping sounded a little more like home. We watched you organize his supplies, label his equipment and make his room comfortable. We watched you obsessively clean, sanitize, sterilize and put on and take off more yellow gowns and purple gloves than we could count to protect our little boy. Even when you may have felt unnoticed or unappreciated, we watched you give your very best to our baby. We not only watched you take care of our son, but you took care of us too. You answered all of my questions. I know I had a lot ("a lot" being an extreme understatement), I know I asked the same questions over and over again and I know I asked questions that didn't always have an answer. Thank you for being patient. Thank you for making me feel as if Will was all that mattered in the world and answering my questions about him was your sole task for the day. I know you had a million things to do and plenty of other tasks to take care of, but you never rushed or made me feel like my questions didn’t matter. Thank you being there when the days and nights were hard. Thank you for showing compassion and empathy when we cried. Thank you for stopping me to pray when we got unexpected bad news. Thank you for the hugs. Thank you for listening when we were frustrated or mad or scared. Thank you for teaching us to take care of Will. Thank you for being patient when it took me forever to help you change trach ties or help with his bath. You could have done it twice as fast by yourself but you took the time to teach and encourage, giving me much needed confidence. Thank you for letting us hold him. We know it took a lot of effort to get him out of his bed and into our arms but you never said no or acted annoyed when we asked. Thank you for making those moments with him a priority because now they are some of our most cherished memories. Thank you for bending rules, sneaking pictures and celebrating with us. Thank you for making much of little victories. Thank you for helping us interpret test results and blood work and labs. Thank you for your opinions, thoughts and wisdom. You may not realize that your words helped us through the most difficult times. To you, it may have just been sharing an experience or a casual conversation, but to us it was advice that we valued and wisdom that helped us have hope and make decisions. Thank you for being positive. Thank you for spending time away from your children to take care of mine. Thank you for being invested. Thank you for working even when you didn't feel good. I know there were days when you were worried about something going on at home or tired from being up with your own baby the night before. Thank you for being there for us even when you needed someone to be there for you. You not only take care of sick children every day, but you take care of their parents too. I told many of you that I could never do your job. I said that because I am in awe of what you do and I know I don't have the capacity to do any of it myself. You come to work every day for a twelve hour shift that lasts way longer than twelve hours. You wake up early, you go home late, you work all day or all night. You work on Christmas and New Years and sacrifice time away from your family to be with ours. You take care of children who are sick, children who are abused and children who are dying. You take care of children who don’t have someone to take care of them. I’m sure you don’t stop thinking about them when you go home. Actually, I know you don’t because I know that you called to check on Will even on your day off. I’m sure at times you feel under appreciated or taken for granted but I can assure you that you are so valued because it takes an extremely special person to do what you do every day. I only saw a small part of your job, I only saw how you took care of my baby, but I know you do so much more than my eyes could see. Words fail to express the appreciation you deserve, but I want you to know that we are grateful. We are grateful that Will knew you. We are grateful that we could trust you when we weren’t there, that you gave Will a chance at life and that you loved him. That is what we are most grateful for, that you loved our baby. You comforted him when he was upset and spent countless hours trying to help him sleep. You stopped by to check on him even on days he wasn’t “your patient.” You teared up when he smiled. You talked to him, smiled at him, dressed him, played with him and changed countless diapers. You were excited to see him, genuinely excited. I can’t tell you how happy it made me when you said how sweet, cute, handsome, strong or amazing my boy was and the best part is that I knew you really meant it. I was so proud when you requested to take care of him and when you were so happy that he was your patient for the day or night. I know it wasn’t easy being in his room. You could barely leave between keeping up with dialysis, feedings, medications and therapies. But you still wanted to take care of him. I know that when Will passed away you were sad too. I know that when you got the news it was hard to go on with your day without thinking about him. I know that when I asked, “Is Will trying to die and we aren’t letting him” you didn’t want to answer me. You knew I was going to ask it, you knew what the answer was and you were heartbroken just like me. You were graceful, caring and compassionate as we watched him take his last breath. You comforted us as we walked to our car to drive home without our baby. You somehow made me smile as I held my son, waiting for him to die. You cried with us, not always in front of us, but I knew that you were grieving with us. You somehow knew exactly what to say. You had to endure his loss in a whole different way than us. You have to walk by “Will’s room” every day you go to work. Maybe by now you have even taken care of another child staying in his room. I don’t know how you do it. I know he is not the only child you have gotten attached to. I know you have held children as they took their last breath and I know you have loved countless children the same way you loved mine. I know you see a lot of them get better - you saw Caroline get better - and I know there are joyful and rewarding parts of your job, but you also experience the sadness and loss and you keep going back. Thank you for going back. Thank you for enduring the heartbreak, devastation, sickness and pain present in the PICU every day and every night. You have studied, trained and learned how to be a nurse, but you are so much more than what you learned in order to earn your degree. I don’t say that to diminish your knowledge in any way, I am amazed at how much you know about medicine and science and the human body, how many questions you can answer and how much knowledge you possess. I say that to emphasize how much of being a nurse comes from you, your personality, your experience, your compassion, your heart. There is no training that can teach you that part. You do so much more than your job requires every day and I will always be grateful that you are part of Will’s life. Thank you for taking care of him, thank you for fighting with him, thank you for loving him. With much gratitude and thankfulness, Will's Mommy These handprints are from the day of Will's passing. His nurse and the hospital Chaplin helped us get his hand prints and foot prints, along with his Caroline's, to keep as a sweet memory of our little boy. I am so thankful for these little hands and all the people who took care of them.
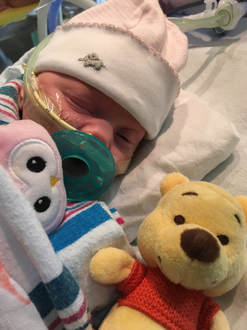
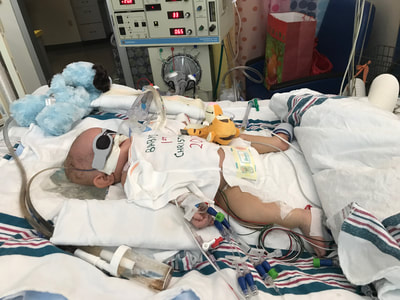
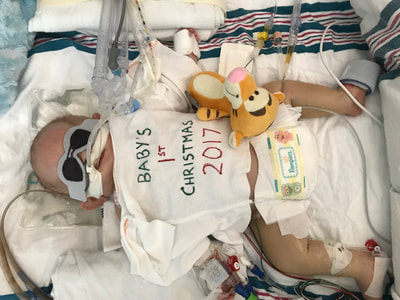
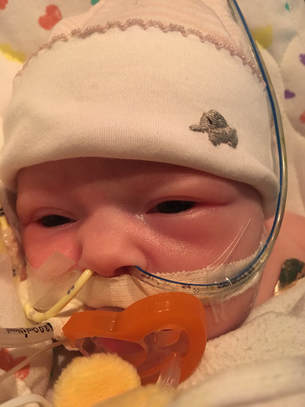
Christmas is a magical time of year - the most magical. All the twinkly lights and decorations and traditions. It is a time of celebration, joy and family. Being in the hospital with two dying babies at Christmas was really hard. Actually, “really hard” isn’t anywhere close to describing it, but there are no words to convey the emotions without actually feeling them. We were supposed to be decorating cookies, reading Christmas stories and sitting around the sparkly tree. We were supposed to get in the car with hot cocoa and drive around looking at decorated houses while listening to Christmas music. Our children were supposed to be wearing matching Christmas outfits and the sweet pajamas I picked out for them months before. Will had a white gown with a Christmas tree on it with green trim that matched his older brother’s pajamas. Caroline’s was pink with white polka dots, same Christmas tree, just like her big sister. I had ordered them in September. They were washed, hung and ready for Christmas time. Neither of our babies ever wore those gowns. Instead they had a white baby shirt, the one with the snaps on the sides, with “Baby’s First Christmas” written in red and green Sharpie by a caring nurse who was trying to make a memory for us. Will’s just lay over his chest because he was too swollen to actually put it on. The week leading up to Christmas gave us a lot of hope. Caroline was improving and every doctor seemed to think she was going to make a full recovery. She was breathing with help from the ventilator but she was taking a lot of breaths on her own and plans were being made to extubate her, meaning she was getting ready to come off the ventilator. She had an MRI done on December 18 that showed she had some bleeding in her brain but it wasn’t extremely concerning. On December 19 she took a pacifier for the first time. This probably doesn’t seem like a big deal because babies take pacifiers all the time, but this was a huge milestone in our minds. Taking a paci meant that she had the reflex to suck and if she could suck then maybe she could eat. I learned from the very amazing speech therapist that sucking, swallowing and breathing all at the same time is very difficult for a baby, even a healthy, full-term baby. She compared it to working out for us. If we were asked to do an intense workout every 2-3 hours throughout the day we would be exhausted. Caroline’s nurse was willing to give the paci a try, even though Caroline was intubated and had a tube in her mouth. She cut the side of the paci so it would go around the tube and to our surprise Caroline took it right away. I remember how sweet it was to watch her with that paci. She was mad about everything and that paci gave her some comfort. On December 21, Caroline got to start having breastmilk through a feeding tube. She responded well to it and was able to get up to her full feedings pretty quickly. She also started being weaned off some of her medications, some of which were narcotics. The side effect of this was withdraw symptoms, so she was fussy, sweaty, sneezy and just overall uncomfortable. It was heartbreaking to see her so upset but also encouraging to see her slowly weaned off all medications. She even weaned completely off the heart medication that they thought she may need to go home with. Her recovery was miraculous. Less than two weeks ago we thought she was going to die. She wasn’t breathing and throwing up blood and the doctors thought she might not make it through the week. Now she was making huge steps forward and fighting to do so. By Christmas Day Caroline was breathing on her own. She had a nasal cannula with some positive pressure and oxygen but was no longer needing the ventilator to breath. My Christmas gift was getting to give her a bottle for the first time since December 6. Getting to hold my tiny baby girl after watching what she had gone through over the past three weeks was one of the happiest moments of my life. She was born, got sick, underwent multiple invasive tests, had tubes, IV’s and lines inserted into her body, used a machine to breath and almost died. She started showing us a lot of her personality during the week leading up to Christmas. She was feisty. She was angry about every tube, needle and anything else that touched her body. She was so responsive and let everyone around know exactly what she wanted or didn’t want. We joked that everyone was a little scared of her, even Taylor and I didn’t touch her much because she got so mad. We would just stand over her little bed and talk to her, sometimes hold her hand, but mostly just try not to disturb her. I hope that she keeps that spirit. It may sound odd because people are always talking about the challenges of raising a strong-willed child, but I hope she stays as strong-willed as she was in that hospital bed. I pray that she isn’t afraid to speak her mind and stand up for what’s right. I think she is amazing and I know she is here for a purpose, just like her brother was. I remember one night during that week so vividly. I was in Will’s room and when I came back to check on Caroline her nurse was giving her a bath and had “Sweet Caroline” playing. We loved this nurse and were always so happy when she was taking care of our babies. It was the same nurse who gave her the paci and the same nurse who loved Will so much. There was no way she could have known this, but Caroline is named after my mom and “Sweet Caroline” is the song my parents did their first dance to at their wedding. She was singing along and it was the first time I had smiled since December 6. I remember really noting that smile. Not because it had been so long since I smiled - it’s not like I had forgotten the feeling of happiness or what it was like to smile. That smile was so significant because in that moment I really felt like Caroline was going to be okay. I knew that she was going to survive, she was going to make it. I smiled because even though she was crying (bath time was not her favorite) there was so much joy and laughter around her. She had been surrounded by fear and machines and anxiety for three weeks and now there was happiness and hope and fun. December 20, 2017 - Caroline with her paci and Winnie the Pooh from her big brother. December 21, 2017 - The last time I held Caroline was around 2am on December 7. She went to get a head ultrasound in the middle of the night and I carried her there and back. I put her down in her bed when we returned to her room and the next morning she was taken to the PICU. This was the first time I got to hold her again. December 25, 2017 - My Christmas present was getting to give Caroline a bottle for the first time! December 26, 2017 - Sweet Caroline, no longer intubated and getting better. The week leading up to Christmas was more positive for Will too. Even though he was in a much more critical state than Caroline, there were small improvements that we put our hope in. I can’t truly describe how Will looked mid-December. His kidneys were not functioning at all and although he had started peritoneal dialysis he still didn’t have the correct catheter and the process wasn’t working well. He was so swollen. At one point we estimated that he had doubled his weight in fluid. Six pounds of fluid. It may not seem like a lot but imagine if you doubled your weight in fluid. He couldn’t open his eyes or move his arms and legs. It’s hard to put into words how I felt seeing him like that. Words like “heartbreaking” and “devastating” aren’t powerful enough to reflect the emotion of it. I desperately wanted to take it all from him, make it better, switch places, make it go away. I couldn’t. Not only were his kidneys not working, but he was on an oscillator for respiratory support. After coming off ECMO he was put on an oscillator because he couldn’t breath on his own. He was sedated and still but his little body was constantly vibrating from the oscillator. He was also on a lot of medications. He had two poles loaded with IV drips. The drips included everything from pain killers to sedatives to heart medications. He was completely dependent on medical technology to live and he was surrounded by it. On December 21, Will opened both of his eyes. I remember standing over him, his bed was raised up high so I had to get up on a stool to see him. He had opened his right eye two days before and was continuing to get fluid off through dialysis. Both of his eyes opened and he looked at me and it was amazing. He had the sweetest, most kind eyes and we hadn’t seen them for weeks. While it was so encouraging to see him awake, there was still trouble with the dialysis. The catheter being used had been placed to help drain fluid from his stomach when he first started swelling. It was more stiff and had less holes than a dialysis catheter, so it kept getting clogged or wouldn’t work if it was not in the correct position. It was frustrating for everyone but he wasn’t stable enough to have the procedure done to put the dialysis catheter in. So he continued being supported and we prayed that he would recover like his sister, that’s all we could do. On Christmas Day I had a conversation with one of our favorite doctors. She was compassionate and honest and promised that she would continue giving Will a chance but tell us if she ever felt it was going too far. She told me that Will would declare himself and we would know if and when his time on Earth was coming to an end. Although he was heavily medicated and dependent on technology, she assured me that there was nothing preventing Will’s heart from stopping if it was going to stop. As she was saying these words to me I was holding Will’s five pound twin sister who was recovering from the same virus that was making him so sick. How could this be happening? He had already survived many days that were predicted to be his last and it felt like he wasn’t done yet. Her words came back to me in the beginning of March when his time on Earth was coming to an end. But not in December, in December he was trying to live. He had shocked a lot of doctors and had a strong will to survive. One of those particularly hard days I was at the hospital with my dad. We had just talked to the neurologist who explained that Will’s brain stem was totally intact and he had brain activity. His neurological status was uncertain and only time would tell what that status would be. After listening to him my dad said how he felt like Will’s name was Will for a reason. He is God’s Will. God made him and God gave him life. God loves him more than any of us could ever imagine. God’s will for Will was good and perfect and right. While the thought of him not being with us was unimaginable, we could trust that God had a good and perfect plan for Will and who were we to tell God what that plan should be. My dad named the group text between me, my husband, my mom and himself “God’s Will” and that is still it’s name today. He belongs to God and God gave us the privilege to be his parents on Earth. I will admit that I don’t fully understand God’s plan, I don’t understand why Will was only here for 96 days and why most of those days were spent in a hospital. Of course I wish I could change it so that Will was still with us. I wish more than anything that he was here now, next to his sister grabbing for toys, rolling over and trying to suck his thumb, just like her. I don't know why that couldn't have been the outcome. I don't know why Will's life on Earth was so brief. But I don’t think I need to or even have to know. If I trust that God is who He says He is, then I can trust that His plan is infinitely better than mine. I can trust that my Will is God’s Will and His will is good and perfect. December 25, 2017 - I have been hesitant to share these pictures of Will because they are so heartbreaking, but I think as I get to January/ February it will show how far he came. He had already been on dialysis for ten days, so he is much less swollen than he was but is still retaining a lot of fluid in these pictures. He is intubated and using the oscillator for respiratory support and has two PICC lines on his right side for IV medications.
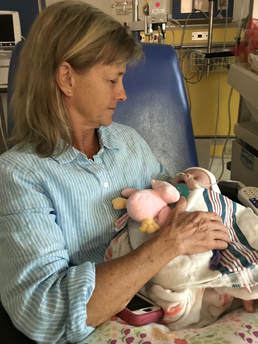
This is an entry from my dad's (Will's Grandaddy) journal from Christmas Day 2017. December 25, 2017 Grandaddy’s Journal Room 312, Wolfson Children’s Hospital Caroline is better. Doctors say today she could be out of PICU in two days. Only thing keeping he in PICU now is Fentanyl, a pain medicine, she has to be weaned from it, has been weaning for the past few days, now reducing rate even more and should be off in about two days. Last time I saw Sweet Caroline before today was December 14th, so it was 11 days ago. She looks so much better today. She looks like a baby. Pink, pretty. She cries quite a bit, wants her pacifier. She is swaddled in a blanket, has a paci with a pink ducky on it. Has a pink Snoopy that Joshua gave her and a Winnie the Pooh. It’s about 11:30 am. Wolfson Children’s Hospital room 311. Candy came here this morning about 5:30 to let Taylor leave the hospital to come to the house for Christmas morning with Joshua and Emma Grace. They had a fun Christmas morning. They were up about 6:00 am, came downstairs to the living room with the Christmas tree soon thereafter. Joshua was excited, he got bumper cars, a robot, a giant Snoopy, shoes and a lot of other toys from Santa. Emma Grace squealed when she ran into the living room and saw all the toys. Santa brought her a little pink baby stroller to stroll baby dolls, and a pink soft chair that looks like a throne for a princess. She also got some shiny shoes and dress up clothes. But maybe her favorite is the Princess Coupe pink car. She likes shoes, jewelry and the car the most. Go figure? She tosses the stuffed animals aside and pays more attention to the car and clothes! She’s 18 months old, so girls are just born this way?! This Christmas is not the one we expected. Caroline and Will were born on December 1st, went home from the hospital on December 4th and were checked in to Wolfson Children’s Hospital on December 6th. They both were rushed to the PICU. It took more than a week for the diagnosis, enterovirus sepsis. Assumingly, they were born healthy but caught a virus in the hospital after birth or after leaving the hospital. It’s unbelievable the damage a virus can do to a newborn baby. It attacks the heart. Both Will and Caroline have been close to passing away more than once. Will has been more severe from the beginning. Today, on Christmas day in the year 2017, 25 days after birth and 19 days in the hospital, Caroline is getting close to being released from PICU but there is no good prognosis for Will. Will continues to be strong. He has lived longer already than the doctors predicted. Today, Candy and I listened to the doctors and nurses do the rounds at 11:00 am. Most of the nurses and doctors were dressed for Christmas, so it was kind of a funny scene to watch a group of elves and reindeer do hospital rounds. The lead doctor said Will’s heart is so weak, it is a muscle that is barely functioning, so it’s not strong enough to power his other organs, especially his kidneys. He has been on kidney dialysis for a little more than one week. It has helped take a lot of excess fluid off of him. The doctor said he had looked like “the Michelin Man.” Because his kidneys had stopped the waste that would typically be urinated out was building up in his tiny body, so he was just becoming big and puffy and misshapen. He just looked so pitiful but the doctor said the fluid buildup isn’t really the concern. The concern is that his heart function is too weak. Regardless of fluid or kidney function, the real concern is his heart. We asked the doctor and she said she has seen children in renal failure come back in one to two months and their heart strengthen but, she said, the concern is: will Will give up before he has a chance or the strength to recover? She didn’t say it but I thought her tone and body language was doubtful. If it was a question about whether Will would give up, I thought, then I am totally betting on Will! From the beginning the thought that kept ringing in my head was “his name is ‘Will’ for a reason.” He is Strong Will. He is God’s Will. Will Power was the nickname I kept using for him. Always and from the beginning, my heart – and the messages I felt and heard as I prayed – kept giving me images of strength and power. I thought, Will has to be incredibly strong. The last time I saw him he was all puffed up, his head misshaped. I prayed at his bed and then Courtney came in and we cried and prayed. We talked to the neurologist, he seemed doubtful although very empathetic and careful in his word choice. For me, it was impossible not to be hopeful that he would recover. How could a baby just born be so sick? Why would God have him live only to die so soon thereafter? Courtney told me that she has said goodbye to him more than once. That was 10 days ago, but Will powers on. I keep thinking: “What is God’s purpose? That’s the right focus, God has a plan. Go with it, lean into it. Miraculously, Will has lived on earth just 25 short days and his life has impacted so many people in so many profound ways. Hundreds are praying for him and his sister. We are living a miracle, God is incredible beyond words. God’s Will is happening inside and all around us, what a joy, what a wonder.” Room 312 is glowing. The light is soft, unusual because the hospital room light is typically bright, intense and cold. But not today on Christmas, its soft and Will glows and it reflects out into the hallway. Music volume is up and playing louder than usual, Christmas music. The nurses have made a shirt for Will and its draped over him with the words “Baby’s First Christmas” in red and green letters. His eyes are covered with a patch and they’ve colored it to look like sunglasses. He lays splayed out, legs and arms to the side, not moving but for the breathing machine. It feels to me like God is here, holding Will in the palm of his hand. I expect God to take him at any second. It’s happening, I think, I hear the trumpets of angels, I hear God calling. I feel Will’s glow and warmth. It’s a meditation, extremely warm. I’m all alone with Will and God in the center of a gigantic hospital. Nobody else is here. I hold Will’s hand and say: “Merry Christmas Will Power, you are a blessing and a gift to all of us.” I love this picture, Lala holding her namesake, Caroline is named after her Lala. We tried to make Christmas morning “normal” but it was hard not to be sad that Will and Caroline were not at home. Emma Grace loved the car, clothes and jewelry. My Sweet Courtney with her Sweet Caroline in the room next to Will’s on her first Christmas.
On the morning of December 15, Caroline had started improving. She was awake a lot over night. She was awake crying, kicking and moving around. She was awake fighting. She was becoming more aware of all the equipment and monitors on and around her and she did not like it. They were starting to talk about when to extubate her, which means she was ready to come off the ventilator and breath on her own. Her numbers were improving, she was urinating and her heart function, while still depressed, was better. Will was not urinating at all. He was extremely swollen, he couldn’t move his arms or legs or open his eyes. We were given the option to try dialysis but there were a few issues. Will was only able to do peritoneal dialysis (as opposed to hemodialysis) because of his size and instability. With peritoneal dialysis, a catheter is inserted into the peritoneum (abdomen) and fluid it instilled through the catheter into the abdominal cavity. It stays in the abdomen for a period of time (called dwell time) and then is drained back out through the catheter. Dialysis does the work of your kidneys, so every time the fluid drains there should be more coming out than going in. Will was not stable enough to go to surgery to get the correct dialysis catheter inserted, so the doctors were willing to try using the catheter he already had, although they thought the chances of it working were small. It was the catheter inserted a few nights before to help drain fluid from his stomach and it was not meant for dialysis. It was stiff and only had a few holes, so the chances of it getting clogged as the fluid went in and out were high. But it was the only option so we said yes, we wanted to try. It seems like over the next few days Will experienced every possible complication with dialysis. Each cycle was supposed to take an hour. 15 minutes to instill, 30 minutes for the fluid to dwell and 15 minutes to drain. I have never lived as hour-to-hour as I did those first few days of dialysis. Did it instill in 15 minutes? If not the catheter was probably clogged. Did he drain? If so, how much? Was he going to have a negative fluid balance for the day? If he had to get blood products or extra medication or electrolytes it could make him have a positive balance because he had more going in than coming out. At the same time we were watching with every diaper change for a sign that his kidneys would start functioning. I hated that little yellow line on the Pampers and wanted it to turn blue so badly. On December 17, there were so many issues with the catheter that they started talking about trying to replace it with a dialysis catheter. The hope was that dialysis would be more efficient with the correct type of catheter so that he could get the fluid off that he so desperately needed. This required surgery. I was in tears as I talked to the surgeon that night. He told me that Will would bleed to death if he did the surgery and because of the risks involved he would not do it. He thought Will had no chance and the thought of my sweet baby bleeding to death in a cold, bright operating room surrounded by doctors was horrifying. I felt like getting the dialysis to work properly was our only hope. Having all that excess fluid was putting pressure on his already weak heart and lungs. That night his blood pressure was so low that the doctor thought he wouldn’t make it to the morning. I had already gone back to my parents’ house for the night and Taylor called me ask what code we wanted Will on. One option is a full code, meaning that doctors will do everything possible to resuscitate the patient. The other option is AND (Allow Natural Death)/ DNR (Do Not Resuscitate). The doctor explained to Taylor that because Will’s heart was so weak, he will not be able to restart it if it stopped, even if he did everything possible. We would just be doing something to Will instead of for him. We decided to tell the doctor not to resuscitate our child if his heart stops. Let my child die. That is what you are saying when choosing this option. It’s not a choice any parent should ever have to make. Let my child die. Don’t try to save him. Part of me felt like making that decision meant we were giving up, but we had to think of the alternative. How could we be so selfish to put our baby through the traumatic experience of aggressive resuscitation when there is no chance of restarting his heart? How could we ask the doctor to hit him for nothing? So again, I tried to go to sleep, thinking that I would not see my son alive ever again. I thought I would receive a call sometime that night from my husband telling me that Will was gone. I thought his heart would stop before I could get to him again in the morning. I was crying, sobbing, with my parents after my two older children were in bed and I remember my dad saying that he would take me back up to the hospital if I felt like I hadn't said good bye. I told him that I had said bye to Will every time I left his side since December 6. Every time I left to pump or go to the bathroom or step into Caroline’s room. There had not been a day where I left, even for a minute, and didn’t know if he would be there or not the next time I saw him. Every night as I put my children in bed I say, “I love you, goodnight and sweet dreams, I’ll see you in the morning.” I have said it every night for five years, with certainty. I have never doubted that I will see my children in the morning. I have never doubted that I will walk into their rooms, usually before the sun comes up, and see them with perfectly messy hair and bright eyes, ready for the day. I never doubted that I would pick them up the next morning and give them a kiss on the forehead and hug them. No parent should ever have to wonder if their child will make it to the next morning. But we did. So far, for twelve nights, I had said goodbye to my babies not knowing if I would see them again in the morning. My only hope was in knowing that I would see them again, just maybe not in the morning. Our God is good. He not only made a way for us to spend eternity in His presence, but He allows us to do it with the ones we love so dearly on Earth. So every night, when it was time to leave, I held Will’s hand and whispered in his ear, “I love you, goodnight and sweet dreams, I’ll see you in the morning.” Not because I was fully confident that I would see my little boy in the morning, but because I was fully confident that no matter what happened I would see him again one day. One of those uncertain nights my husband texted me this, “Whether in life or death, God will be glorified in Will and I take great sorrow and yet joy in knowing that.” Will didn’t die that night, I saw him the next morning and many more mornings after that. Another time that Will lived when, according to medical standards, he shouldn’t have. Another chance at life. Another display of strength from our little baby. Another miracle. This was Caroline around mid/late December. She was intubated, the tube going into her mouth is attached to the ventilator and the tape over her face is helping to keep it in place. The yellow tube is her feeding tube so she could get breastmilk since she couldn't eat yet. It is hard to look back at pictures of her and see how sick she was, but looking at her today shows just how far she has come! Below are pictures of four-month-old Caroline. She is healthy and strong. She rolls over, grabs for toys and even had her first trip to the beach. She is the happiest baby I have ever met - she laughs at everything and just looking at her makes her smile. I am overjoyed at every milestone she reaches but also heartbroken that her brother isn't here to reach them with her. What a sweet blessing she is! I woke up the morning after Will came off ECMO (December 13) and he was still alive. I had so many emotions I don't really know how to describe how I felt - relief, disbelief, shock, fear, sad, numb - I was feeling everything and nothing all at the same time. Before going to the hospital, I went to Will's older bother’s pre-school Christmas performance. They retold the story of Jesus’ birth and Joshua was one of the three wise men. The school was live-streaming the play on Facebook, so Taylor was able to watch from the hospital room. I imagined my babies listening to their older brother sing. I pictured them as four year olds dressed as a little wise man or angel in their play. I thought of them signing about Jesus being born and God’s plan for salvation through His son. I cried. I tried to hide it but I couldn’t help mourning the loss of seeing them like their older brother. Even though they were both still here, I knew there was a very real possibility that I may not see my babies make it to four years old. Just 12 hours before I was told that Will was going to die and a few days before I was told that Caroline was in a life-threatening condition, that she may or may not make it another week. Not having my babies seemed like more of a reality than having them. I knew that I may never see either of my twins sing a Christmas song, dress up in a costume, perform on a stage, go to school, walk in a line with the rest of their classmates or beam with pride when they see their family watching from the audience. I cried because I imagined them hearing those sweet children singing about Jesus and knew that it may be the only time in their lives that they ever hear singing. It may be the only time they hear the story of Jesus’ birth. It may be their only Christmas. After the play I went back to the hospital. Will was on the highest level of support and medications to keep his heart going. If he started having low blood pressure or his heart stopped there was nothing they could do about it. It was the eighth day in a row that I thought my babies were going to die. Eight days of not knowing why they were sick. Eight days of praying desperately that God would heal them. We had a routine by day eight. I would spend the night at my parent’s house with our two older children and go to the hospital during the day, giving Taylor a chance to have a break and spend time with the older two as well. Every night I would get up to pump every three hours and text Taylor to check on the babies. This is the conversation that we had the night of December 13: Me: “Tell him I love him.” Taylor: “I do all the time” Me: “I just want him so badly. I just want him to be strong and healthy and get better.” Taylor: “Me too. More than anything. Ever since we came here I can’t get the lyrics of “It Is Well With My Soul” out of my head. We love him so fiercely but I want to trust in God’s best for him. Just like your dad said, he is God’s Will and God blessed us by allowing us to be parents of the sweetest boy.” Me: “You’re right, those lyrics have been in my head too. He is already a miracle and I pray that God heals him. I just love them both so much and I can’t imagine not having them, but I know God has a plan for them both and trust whatever that plan is will bring Him the most glory. Please tell them both goodnight and mommy loves them” Taylor: “I will my sweet wife” Me: “And make sure they stay warm” Taylor: “They are both snuggly” December 14, 2017. We had been in the hospital with our babies for nine days and we finally got a diagnosis. Enterovirus. I thought I had never heard of it but I actually had. I had never heard the word “enterovirus," but when the doctor explained it to me, I knew what it was and I had most likely had experience with it. He said that it is a very common virus. One that we all have at some point in our lives. It has a wide range of symptoms and effects everyone differently. Some people could have a mild headache, others have symptoms of the “common cold” and some may never really have any symptoms at all. That was scary to me. Someone could have had this virus that is killing my babies and may not have even felt sick. But how? How did they get infected with this virus? We didn’t parade them around the mall or take them to the playground or have visitors at the hospital or when they came home. We are the overly cautious parents but even with all our protection they were still exposed. It could have been anyone - a doctor or nurse, the pediatrician or someone who brings in the trays of hospital food. It could have been one of us. Everyone thinks babies are so tough and resilient. They are in a way, but they are also so fragile and so vulnerable. A virus that is super common, a virus that everyone has at some point during their lives, was causing their bodies to literally shut down. The resident explained to me that since babies have such immature immune systems it is not uncommon that their bodies would react to a virus like this. They had some reserves that they received from me before birth and maybe some antibodies from the few days of breastmilk they took in, but that ran out very quickly as their bodies tried to fight the virus. When they came into the hospital they had literally zero white blood cells. Their bodies had used everything they had to fight the virus and had nothing else, so they were shutting down. Multi-organ system failure. That’s what it’s called when your body stops working. Heart, brain, kidneys, liver, lungs - they were all failing. We finally had a diagnosis, so it was positive in a way because we knew what was making our babies so sick. However, since it was a virus, it changed nothing. Its not like we got a diagnosis and then there was some other treatment or cure for them. There is not a cure for a virus, you support the body until it “runs its course.” Our babies were being fully supported, so the question was could they make it until the virus runs its course and could they recover from the damage done from the virus. Caroline did and her brother did not. At this point, I couldn't take a picture of Will. Whether he lived or not, I knew that I didn't want to remember the way he looked. I wanted to take all the pain from him, I wanted so badly to just switch places with him. Since I couldn't do that, I wanted to make sure he knew we were there, so I held his hand, rubbed his head and talked to him as much as I could.
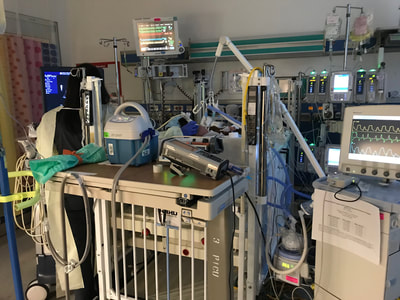
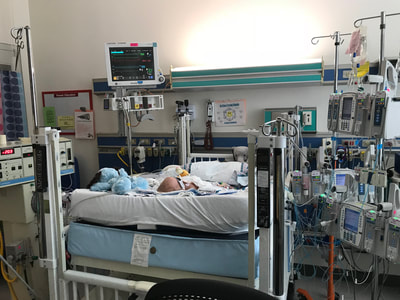
Extracorporeal Membrane Oxygenation. Hearing that your child needs to be on this machine, also know as ECMO, is not what you want to hear. I had never heard of this machine before, but on December 11 the doctors told us that Will needed to be put on ECMO or his chances of making it even a few more days was pretty much none. This machine is used for patients with life-threatening heart and/or lung problems. There is a large plastic tube inserted into the blood vessel in the patient’s neck which takes the blood out of the heart and into the ECMO machine. The machine oxygenates and cleans the blood before it is pumped back into the body. When successful, ECMO will help support a patient while doctors can treat the underlying problem and it can be a life-saving machine. However, like with anything, there are risks. On the morning of December 10 neither baby was showing any signs of improvement. Caroline was in critical condition after the pulmonary hemorrhage and we still had no test results indicating why they were so sick. Caroline was on an oscillator and Will on a ventilator for respiratory support and both of them had very poor heart function. They both had enlarged livers, poor kidney function and Will also had an enlarged spleen. Both babies were starting to swell due to poor kidney function but Will was retaining more fluid than his sister. That night the doctor put a catheter in his stomach to help draw out more fluid. We were told that if they didn’t put the catheter in he may not make it a few more days because the extra fluid puts pressure on his heart, which was already weak, and on his lungs, making it harder to breath. Will had a really hard time overnight. He stopped draining through the catheter, his kidneys stopped producing any urine and his heart was not squeezing well. I had spent the night at my parent’s house with our two older children and this is the text I got from Taylor when I woke up in the morning, “He (the doctor) just told me he is extremely concerned for Will and doesn’t want us to be blindsided if something happens. Just get here as soon as you can, the doctor said if he goes into a heart arrhythmia or if his heart stops he doesn't know that they can get it going again.” Two days before I thought I would show up to the hospital to find that my daughter was gone, today it was my son. On December 11, the doctors started talking about putting Will on ECMO. It was the only thing that the PICU team thought would give him a chance, even if it was a small chance. The procedure to insert the tubes and begin the process went smoothly and we had great hope that this would give his little body the chance to rest and recover. When your child is on ECMO, there are a lot of people, medications and equipment involved. There is a PICU nurse and an ECMO nurse present at all times in the room. Will’s first few hours on ECMO went well, he was responding to the machine and everything was working the way it was supposed to. Then he had a head ultrasound. One of the major risks with ECMO is bleeding, especially for little babies. The patient needs a large dose of blood thinner for the process to work and Will was already having issues with his blood coagulating correctly. The head ultrasound showed that his brain was bleeding. I was sitting with Will on the night of December 12. His bed was raised up high, so I had gotten an office chair that the nurses use and adjusted it up to the highest position so I could sit next to the bed and hold his hand. That night Taylor had gone to our daughter’s Christmas performance so I was alone with the babies and was planning to go back to my parents' house when Taylor got back from the show. Will’s room was positioned at the end of the hallway and I remember glancing over to see Taylor coming down the hallway. He wasn’t supposed to be back for a few hours and I immediately got huge lump in my throat. I knew something was wrong. Without even saying hello I blurted out, “What are you doing here?” He acted surprised, like he thought I should know something that he didn’t. He told me that right as he arrived at the performance the hospital Chaplin had called him and said that the doctors needed to talk to us and he needed to come back. I had no idea that the Chaplin had called Taylor or that anything was wrong. Minutes later we were taken down the hallway to a meeting room and the whole team of doctors and nurses came in. They explained to us that Will had to come off ECMO because of the brain bleed. He had been on it less than 24-hours and the positive effects of ECMO had not even begun to take effect. The doctor thought that Will may have a short time after being taken off the machine, but made it very clear to us that either his heart would stop or his lungs would collapse within a few minutes or hours. There was nothing else they could do. Everyone left the room and prepared to disconnect Will from ECMO as we crumbled, completely devastated. Taylor and I were both sobbing and I remember thinking so many things but all I could say was, “I don’t want him to die.” After a few minutes alone, we went back to Will’s room to be with our baby for what we thought were going to be his last few minutes, possibly hours, on Earth. I pulled the tall chair back up to the bed to hold his hand and Taylor stood next to me near his head. Through blurry eyes I kept glancing at the monitor then back down at Will. Lots for doctors and nurses were gathered in our room doing the same thing. After about thirty minutes I asked the doctor when they were going to disconnect him from ECMO. “He’s all on his own,” he replied, keeping his eyes fixed on the monitor. It felt like everyone was just waiting for him to die, there was a certainty that it would happen any minute. But as the minutes went past, the room got more and more empty. Will’s heart never stopped that night, it kept going the next day and the next and for almost seven more weeks after that. His lungs never collapsed, ever. No one could believe it. It was a miracle. He is a miracle. A few weeks later I was talking to the same doctor who was there that night and he brought up some things that he thought Will would never be able to do. Will was doing fairly well at that point, he was pretty stable and just needed time to grow and get stronger until we could see what his path was going to be. The doctor was mentioning things like Will would probably never drink from a bottle and he may never walk or talk, all things that were unknown and far into the future. I reminded him that Will had already done a lot of things that no one thought he could, specifically he lived through something that no one thought he would. He replied saying that it just goes to show how little control we have. We feel like we are in control with all the medication and equipment and support available, but really, even with all the things we can control, we are totally out of control. Even with all the medical support possible, God could have taken Will despite all of our efforts. God could also keep his heart beating despite all of the reasons why it shouldn’t. He is the Creator and Giver of life. That night He gave Will life. He gave us seven more weeks to spend with our baby. He gave us hope. He gave us a miracle. This is what Will's room looked like after he was taken off ECMO. The large machine on the left is the oscillator, which he was on for respiratory support. The black screen mounted on the wall is the monitor that we were constantly looking at that night to watch his heart rate and blood pressure as we were waiting to see if they would start dropping. On the right are two IV poles with medication drips going into Will's PICC lines, he had one in his leg and one in his arm at this point because he required so many medications. You can tell that his head is swollen from the top as was the rest of his body.
After both babies were admitted to the PICU, they were soon moved to rooms next to each other. There was a sliding door between the rooms so we could easily go back and forth between them. By December 8 (two days after taking the babies to the ER), it seemed like they had undergone every test imaginable. They had blood samples taken, head ultrasounds, EEG’s, X-rays and echocardiograms. There was still no explanation and neither baby was showing any signs of improvement. They had similar symptoms but they were starting to differ in a few ways as well. On December 8, Will had an arterial line inserted to consistently monitor his blood pressure because his heart function was so low. He also had a few episodes of his heart rate increasing. Clinically, he looked and seemed to be much sicker than his sister, but Caroline’s numbers were worse than his. After 24-hours in the PICU, she was being fully monitored just like Will. She had a PICC line inserted as well to get medications and draw blood, she had a nasal cannula with oxygen to assist with breathing and she was on IV fluids because she couldn’t eat. Sometime in the early morning on December 9, Caroline started to get worked up and became very agitated. Taylor had spent the night at the hospital and I spent the night at my parent’s house with our two older children. I was planning to go to Breakfast with Santa with them that morning before I went back to the hospital. As we were getting ready I got a text from Taylor that said, “Something bad is happening to Caroline.” I called him immediately and he described our baby girl screaming, crying, coughing and throwing up blood. I sat on a chair in my parent’s family room, sobbing. Taylor was silent on the other end. “You should come here,” he finally said. My mom drove me to the hospital and I was certain that I was walking up to find that my baby girl was gone. Once I got to her room there were still a lot of doctors and nurses taking care of her. It was complete chaos and panic. I sat in a chair right outside her door, Taylor stood next to me and the resident explained that Caroline experienced a pulmonary hemorrhage, bleeding from the lungs. They didn’t know what had caused it, but she was intubated and put on a ventilator immediately. We were told that she was in a life-threatening condition. Over the next week or so we would know if this event would take her life or not. When we got to see her again later that morning she was sedated, breathing with help from a ventilator and motionless. That night she was switched from the ventilator to an oscillator. An oscillator is a type of ventilator, they are both used to assist with breathing by getting oxygen into the lungs and removing carbon dioxide. A ventilator works by physically inflating and deflating the lungs, so the patient has chest rise and fall just like when they are breathing all on their own. An oscillator keeps the lungs open with positive pressure and vibrates quickly to remove gases. It is gentler on the lungs, so the decision to switch Caroline over was to protect her lungs since they were so delicate from the hemorrhage. An oscillator is very loud and has a continuous, systematic hum as it delivers hundreds of tiny breaths. It is a large, outdated looking machine and is used for very critical patients. When I saw her the next morning she was being supported by the oscillator, her little body was swollen because her kidneys were not functioning well and she was heavily sedated. I thought she was going to die. The next morning Taylor remembers the doctor waking him up to explain to him what critical condition Caroline was in. This particular doctor was our very favorite from the first time we met him. He saved both of our children so many times, was willing to give them a chance and communicated with such compassion. During every procedure and emergency we never saw him as worried as he was that day. He saved Caroline’s life on December 9, Taylor said her blood was all over him and he did everything in his power to make sure she survived the pulmonary hemorrhage. He was very concerned for both of our babies and told Taylor, “if you are a praying man, you should pray.” So we prayed. We prayed first for what we wanted. We wanted our babies to be healed. We wanted our babies to be healthy. We wanted them to fully recover. Quickly. We wanted to know what made them so sick. We prayed that they would get better. We also prayed for God’s will. We prayed that God would do whatever brings Him the most glory. We declared God’s sovereignty and we prayed that He would help us to trust Him, no matter the outcome. We prayed knowing that prayer is not some magical way to get what you want from God, but that it is our way of communicating with our Heavenly Father. We prayed knowing that God uses our prayers to carry out His plan. We prayed knowing that God is good no matter what. We prayed in confidence that God could hear us and that He knew the desires of our hearts. We prayed in a way we never have before - desperately, urgently, continuously. Photos by Brooks Wilder Photography.
We are so excited to share a little bit about the first baby that we have been able to support in memory of Will! We started this foundation with the simple idea of having a way to honor Will by helping other children. We are grateful that we were able to help beautiful baby Avery receive a heart procedure through Patrons of the Heart. This is an organization founded by Will's cardiologist, Dr. Ettedgui, and his wife. They have already helped so many children in the past 13 years and we are are so thankful that they allowed us to be a small part of Avery's journey.
Avery and her mom are from Grenada and traveled to the United States for the first time last weekend. We got to meet them the day before Avery's procedure and we loved getting to spend a few hours with this sweet family. I have tried to imagine what Avery's mom must feel like - she is a young, first time mother with a baby who is in need of a medical treatment that is not available in her country. She traveled all by herself (a 12-hour flight with an infant!) to a country she has never been to where there is no one she knows to get her child the help she needs. She kindly agreed to meet our family and I'm sure it was overwhelming to have all five of us greet her! We walked to a local park and spent time getting to know her and Avery and hearing their story. I was so amazed by her strength and courage as she described their past few months of hospital stays, getting a diagnosis and finding a way to treat her daughter. Avery is such a sweet, calm baby and she is so beautiful! Our two older children loved her and thought it was funny that Caroline is bald while Avery had so much hair. It was so special for us to see our children with Avery and know that they will be a part of seeing how Will's life impacts other children. Joshua (5) was so happy that Caroline had a "baby friend" and he prayed for Avery's surgery and has asked about her every day since we met her. I am confident that God will use Will's life to impact others because I know that it has already impacted us, his family. My children will get to help others, meet people from all over the world and pray for them. I am thankful for that. We are so happy that Avery's procedure went well. She will recover for a little while longer in Jacksonville before going back to Grenada with the rest her family, who I'm sure will be so happy to see their healthy little girl! We will continue to pray for Avery and hope that she is the first of many children that we can support in memory of Will! |
Our MissionOur mission is to children from developing countries receiving heart treatment in Jacksonville, FL. Archives
January 2023
AuthorMy name is Courtney Hughes and I am Will's mommy. I am happy that you are here to read Will's story and make a difference with us! |